When Feeding Struggles Point to Something Structural
You know something is not quite right.
Feeding should not feel this hard. You have tried everything your lactation consultant suggested, adjusted the positioning, tried a shield, given it more time. But your baby still struggles to stay latched. You hear a soft clicking sound. Nursing sessions stretch past forty minutes and leave you both worn out. Weight gain has slowed, and feeds that were supposed to bring closeness have started to feel like something you are bracing for instead.
None of this is your fault. And you are not imagining it.
When feeding remains difficult despite good support and consistent effort, the cause is often structural. A tongue tie can quietly prevent your baby from forming the deep, comfortable latch that makes nursing work the way it should.
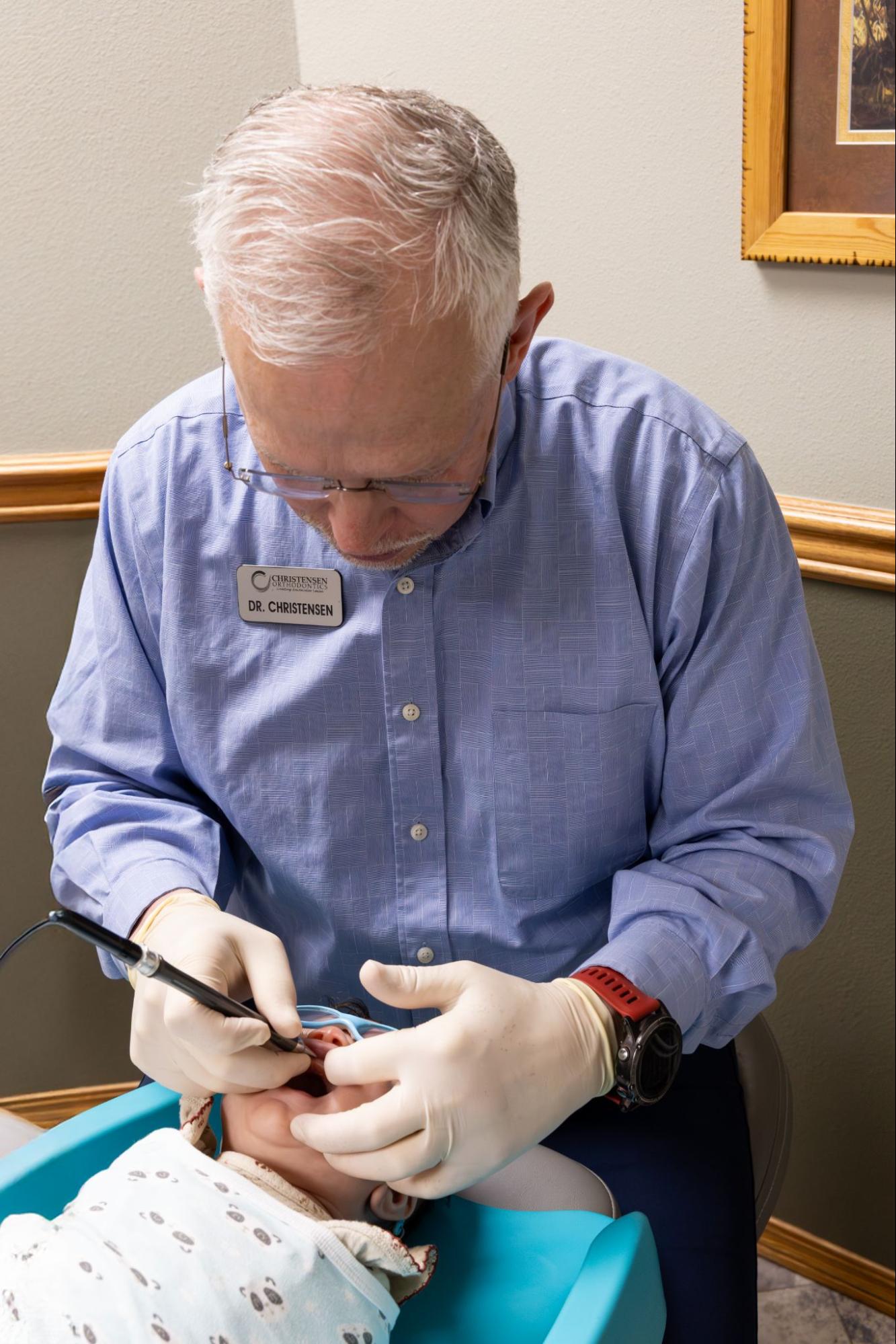
Eddieka Christensen, Dr. Christensen’s wife and a certified breastfeeding counselor, works alongside our clinical team with infants and families going through exactly this. She understands the emotional weight of feeding struggles, not just the mechanics, and she has walked with many mothers through the uncertainty of not knowing why something so natural feels so difficult. When you bring your baby in, she is part of the conversation from the beginning.
What Is a Tongue Tie?
A tongue tie, called ankyloglossia, occurs when tissue beneath the tongue restricts its normal movement.
The tongue is designed to lift upward and cup against the roof of the mouth during feeding. That upward seal creates the suction that draws milk efficiently. When the frenulum is too tight or too short, the tongue cannot elevate fully. Instead of cupping upward, it presses forward or stays low. Milk transfer slows. Your baby works harder for less.
Sometimes the restriction is visible near the tip. This is called an anterior tongue tie. In other cases, the restriction lies deeper, beneath the surface. This is a posterior tongue tie. Posterior ties can be difficult to see on casual inspection, but they can limit function just as significantly.
We evaluate based on what the tongue can do, not what the frenulum looks like.
Signs of Tongue Tie in Newborns
- Painful or shallow latch
- Clicking sounds during feeds
- Frequent unlatching and re-latching
- Prolonged nursing sessions with poor milk transfer
- Fatigue during feeding (baby falls asleep at the breast before finishing)
- Slow or inconsistent weight gain
- Gassiness, fussiness, or reflux-like symptoms
- Maternal nipple damage or recurring mastitis
Not every feeding problem is caused by tongue restriction. But when these signs cluster together and persist despite support, the tongue should be evaluated.
Why This Matters Beyond Feeding
Here is something most parents are never told:
The roof of your baby’s mouth is also the floor of their nose.
When the tongue rests fully against the palate (which it is designed to do) it provides gentle, continuous pressure that helps the upper jaw widen naturally as your child grows. As the palate widens, the nasal airway widens with it. This is how the body builds space for lifelong nasal breathing.
Roughly half of all facial growth happens by age two.
If the tongue cannot reach the palate during this window because of restriction, that natural widening stimulus is reduced. The upper jaw may develop narrow. The nasal airway may remain small. And a pattern can begin (mouth breathing, disrupted sleep, compromised growth) that becomes harder to redirect the longer it continues.
Early evaluation does not obligate treatment. But it provides clarity during the period when growth is most responsive.
How We Evaluate Infant Tongue Tie
We do not diagnose tongue tie by appearance. A visible frenulum does not automatically mean restriction, and a frenulum that looks normal can still limit function.
Our evaluation focuses on:
- Tongue elevation: Can the tongue lift fully to the palate?
- Latch mechanics: Is there a deep, stable seal or a shallow, compensated latch?
- Suction strength: Can your baby maintain consistent suction throughout a feed?
- Milk transfer: Is feeding efficient, or is it prolonged and exhausting?
- Resting tongue posture: Where does the tongue sit when not actively feeding?
We collaborate with lactation professionals to understand the full feeding picture before recommending any intervention.
Treatment is considered only when measurable functional limitation is present.
When We Recommend a Tongue Tie Release
A frenectomy is recommended when evaluation confirms that restriction is meaningfully limiting tongue mobility and affecting feeding, growth, or early airway development.
The goal is not to "clip a tie." It is to achieve a complete functional release, meaning the tongue can elevate fully to the palate without residual restriction at the base.
How the Procedure Works
We use CO₂ laser technology, which allows precise release of restrictive tissue with minimal collateral damage to surrounding structures. The laser provides exceptional visibility and control, allowing access to deeper fibers that scissors or cautery may not reach as cleanly.
For infants, the procedure itself takes seconds. Most babies resume feeding shortly afterward.
Parents can expect:
- A brief procedure with minimal bleeding
- Feeding attempted within minutes of release
- Mild fussiness for one to two days, resolving quickly
- A healing site that remodels over several weeks
Your Role After the Release
This is the part most parents are not prepared for, and it matters as much as the procedure itself.
After release, gentle stretches are performed three times daily to maintain separation at the release site while it heals.
Your care team will show you exactly what to do. The stretches are brief, and most babies tolerate them well after the first few days.
The goal is to preserve the full range of motion achieved during the release so the tongue can begin doing what it was always meant to do: rest against the palate, support feeding, and guide early jaw development.
When We Do Not Recommend a Release
- The tongue can elevate fully to the palate without strain
- Feeding is efficient with appropriate weight gain
- Latch is stable and sustainable
- There is no measurable impact on function or early growth patterns
A prominent frenulum is not the same as a restrictive frenulum. Our responsibility is to intervene only when restriction is meaningfully affecting your baby, and to leave anatomy alone when it is working as designed.
What Comes After the Procedure
For many infants, a successful release combined with consistent post-procedure care resolves the feeding struggle that brought the family in.
As your child grows, we monitor how jaw development, tongue posture, and breathing patterns unfold. Some children develop beautifully from here. Others may benefit from evaluation again around ages three to five if structural or airway concerns emerge.
The earlier we understand what is happening, the more options we have — and the simpler those options tend to be. If your baby is struggling to feed and you have been told it will get better with time, it is worth asking whether airway structure is part of the picture. Our Lewiston, Idaho practice is here to evaluate, explain, and help you decide what makes sense for your child. We welcome patients from throughout North Central Idaho and from across the United States, Canada, and beyond.

